Building a sustainable ecosystem for phage therapy
Exploring how Phage Australia must embrace novel regulatory pathways, as yet undefined reimbursement mechanisms, supply chain and manufacturing/distribution/logistics and completely new clinical services to ensure sustainability.
Over last 4.8 years, led by Jon Iredell, Australian clinicians, scientists and regulators have been working collectively to implement bacteriophage therapy in Australia. This work has culminated in the creation of “Phage Australia”, and its AusPhageNet Clinical and AusPhageNet Bio network. As we seek additional funding from MRFF Frontiers Stage 2, philanthropy and venture capital to establish an Australia-wide resource, here are some of my reflections.
I have previously outlined the importance of balanced co-investment from public and private sectors in a peer-reviewed biobanking discussion paper [^1]. In the last few years, we have linked phage characterisation to existing publicly funded bacterial pathogen surveillance systems and the standardised monitoring of phage therapy in public hospitals here in Australia.
Now, to ensure sustainability, we must define commercialisation pathways. The biobanking arm of Phage Australia must embrace novel regulatory pathways, as yet undefined reimbursement mechanisms, supply chain and manufacturing/distribution/logistics and completely new clinical services.
We commissioned Deloitte for a market sounding analysis, funded by NSW Health. This revealed that risk-averse investors will likely be unwilling to support investment at this stage. Thus, over the last 12 months (MRFF Frontier Stage 1 funded), we were able to crystalise ideas and address the main issues, which I will outline here.
1. Robust manufacturing and distribution (including supply chain and biobanking).
We collaborate with UNSW Recombinant Products Facility (Chris Marquis, Helene Lebhar, Ali Khalid) for phage purification processes (see Jessica Sacher’s articles [^2]), Citizen Phage Library (Ben Temperton) and Phage Australia network for potential phage supplies, and our own testing on distribution/stability testing of Pae7 phage (see Stephanie Lynch’s article [^3].) We have already produced and distributed a batch of clean home-grown phages to all our partners for testing. I am acutely aware of the effort and investment needed for a biomanufacturing and bioprocessing plant dedicated to phage.
We have demonstrated strong feasibility of networked biobanking at state level (NSW Govt funding for Pathogen [^4] and Phage [^5] biobanks, WA health department endorsed implementation task force); national level and international level, i.e., Israel Phage Biobank (Ronen Hazan, Ran Nir-Paz), LysenTech (South Korea, Heejoon Myung), Denmark (Lars Hansen, Nikoline Olsen), Belgium (Jean-Paul Pirnay, Pieter-Jan Ceyssens, Rob Lavigne) etc.
In the last 12 months we have demonstrated operational logistics in terms of phage exchange at state, national and international level, standardised workflows for sample submission and patient screening, genomics sequencing, patient isolate and phage screening under STAMP [^6] and standardised data curation (see Jan Zheng’s articles [^7]) to produce Australian Phage Passport (to be published soon).
It is important to note that the availability of diverse high-quality phages is facilitated by our bioprospecting programs (Stephen Stick [^8], Anthony Kicic, Trevor Lithgow, Jeremy Barr) and our national and international linkages. The accurate representation of bacterial strains that is our stock-in-trade enables us to identify which phages we need on the shelves and which phages can be lower volumes, as well as which ones can be available in a few days or a week. This sets us apart from all of our competitors and is the power of our national network.
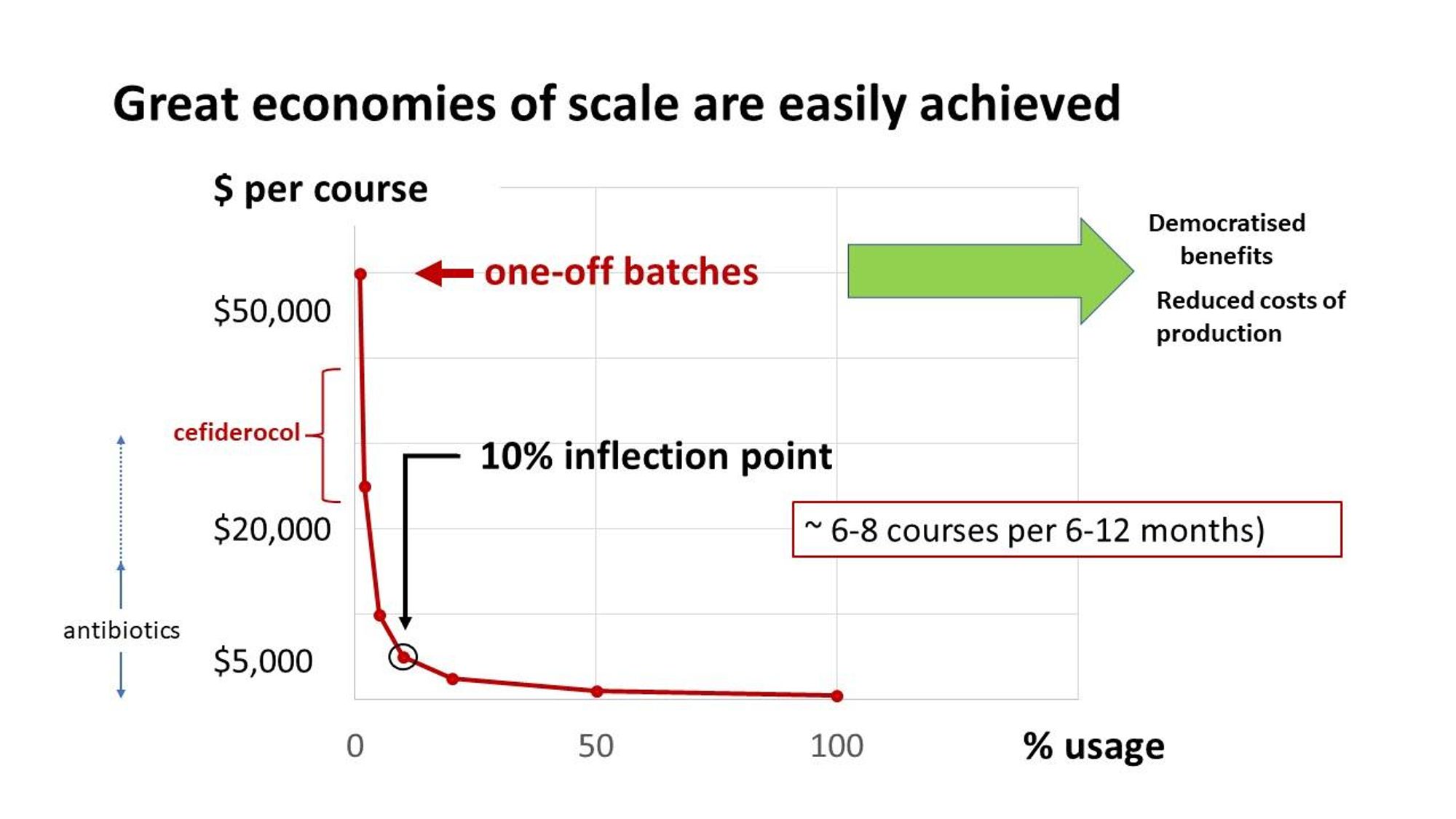
Here, we present our calculations on phage production [^9]. Phage production is a growth process. We have reconciled with the fact that a small batch costs almost as much as a large batch, and efficiencies of scale are very important. For a ~$60,000 AUD GMP-grade one off batch of ~1,000 doses (~30 courses) means we can produce phages for about the cost of a modestly priced antibiotics. Accounting for a clinical trial with 50% wastage, this is well beyond the inflection point for economies of scale.
[^1]: Phage Biobank: Present Challenges and Future Perspectives. RCY Lin, JC Sacher, PJ Ceyssens, J Zheng, A Khalid, JR Iredell & The Australian Phage Network. Current Opinions in Biotechnology https://doi.org/10.1016/j.copbio.2020.12.018
[^2]: https://www.phageaustralia.org/blog/phage-batch-results, https://phage.directory/capsid/phage-making-first-results
[^3]: https://phage.directory/capsid/phage-shipping-around-australia
[^4]: NSW Pathogen Biobank, Jon Iredell, Ruby Lin, Tania Sorrell, Dominic Dwyer, Wieland Meyer, Sharon Chen et al. $100k awarded, 2019-2023.
[^5]: NSW Phage Biobank, Jon Iredell, Ruby Lin. $100k awarded, 2020-4
[^6]: https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?id=382817&isReview=true
[^7]: https://phage.directory/capsid/how-to-organize-phage-biobank-data; https://phage.directory/capsid/how-to-name-a-phage; https://phage.directory/capsid/how-to-track-phages
[^8]: “On country” bioprospecting, phage naming in language, rapid through-put susceptibility testing; Ng RN, Grey LJ, Vaitekenas A, McLean SA, Rudrum JD, Laucirica DR, et al. Development and validation of a miniaturized bacteriophage host range screening assay against antibiotic resistant Pseudomonas aeruginosa. J Microbiol Methods. 2021;190:106346.
[^9]: Based on quotes from third party GMP-phage production and hospital statistics.
2. Effective regulatory pathways.
Facilitated by NSW Health (Tony Penna, Laura Collie, Julia Warning and Sian Hope), we are working with representatives from TGA (Therapeutic Goods Administration) and OGTR (Office of Gene Technology Regulator) to regulate phage therapy in Australia. We will share this in due course.
We have established a clinical network and a nationally approved protocol to regulate phage therapy under the clinical trial framework i.e., Safety and tolerability of Standardised Treatment and Monitoring of Phage therapy (STAMP) in adults and children (Australia and New Zealand Clinical Trial Registry: ACTRN12621001526864 [^10]). This is endorsed by ASID (Australasian Society for Infectious Diseases), ASID paediatric infectious diseases arm (ANZPID), CFA (Cystic Fibrosis Australia) and TSANZ (Thoracic Society of Australia and New Zealand).
Standardised treatment protocols endorsed by expert groups together with clinicians and nurses, training & education are an integral part of Phage Australia’s value proposition. To note, this will be developed further towards “Phage Therapy for Critical Infection”, similar to the S100-style training i.e., Critical Care Short Courses at both Westmead and the Alfred that have been self- sustainable for over a decade. Furthermore, we have designed a Phage Therapy Education Package for scientists and consumers (Sian Hope, Ruby Lin) that is waiting to be signed off. I will detail the importance of industry participation in training workforce, specifically PhD students [^11], in the next instalment.
[^10]: https://www.anzctr.org.au/Trial/Registration/TrialReview.aspx?id=382817&isReview=true
[^11]: https://www.science.org/content/article/controversial-plan-brings-ph-d-students-biotech-training
3. A roadmap for clinical Pathways and the patient journey.
In collaboration with NSW Health (Sian Hope, Julia Warning, Laura Collie), we mapped out the patient journey for phage therapy in comparison to patients being treated with antibiotics only at a public hospital, e.g., Westmead Hospital. To note, Jon Iredell and Ameneh Khatami remain the only two clinicians in Australia with phage therapy and therapeutic monitoring experience (see our publications on Phage Australia website), as well as the process of phage-pathogen matching towards production of a purified phage for intravenous administration.
A health implementation plan for phage therapy in the clinic (Manisha Yapa) will ensure that the most efficient implementation of this new therapy is understood well in advance of the rollout once it is ‘main streamed’.
Health economics are outlined below, and phage production cost is outlined above.
4. Cost-effective payment and reimbursement pathways.
We commissioned HTAnalysts [^12] to map out in the first instance feasibility and impact of phage therapy for AMR (antimicrobial resistance) sepsis [^13] and prosthetic joint infection (PJI).
Substantial savings are made with phage therapy, i.e., $122.8M over a 6-year window for PJI and $67M for sepsis (over 3 years). See link to the reports. Briefly the findings are outlined here.

The key findings for AMR sepsis are (as outlined in the report [^amrsepsis-pdf]):
- If all patients across Australia with AMR sepsis (2,461 patients) were treated with bacteriophage therapy, the total savings over 3 years were estimated to be $67.0 million corresponding to an average saving of $27,239 per patient.
- If all patients across NSW with AMR sepsis (782 patients) were treated with bacteriophage therapy, the total savings over 3 years were estimated to be $21.3 million.
- The total direct savings (healthcare related savings) were $21.8 million, all of which was paid for by the government.
- The total indirect savings (non-healthcare related savings) were $45.2 million, most of which was paid for by patients (63%) followed by employers (20%) and the government (17%).
- Length of stay for patients with AMR sepsis is estimated to be reduced by an average of 7.6 days per patient.
- Resolved infection from bacteriophage is estimated to reduce average time off work by 13.2 months per patient, reducing potential lost income for patients who were previously working prior to their hospital admission.
- Over the 3-year time horizon, 31 patients with an AMR sepsis infection would avoid long term disability (classified as not returning to work within 3 years of discharge), resulting in the reduction of home care, disability support, and the need for a primary caregiver.

The key findings for PJI are:
- If all patients across Australia with prosthetic knee and hip infections (2,573 patients) were treated with bacteriophage therapy, the total savings over 6 years were estimated to be $122.8 million in 2022 corresponding to an average saving of $47,736 per patient over 2 years [^pji-pdf].
- If all patients across NSW with prosthetic knee and hip infections (818 patients) were treated with bacteriophage therapy, the total savings over 6 years were estimated to be $38.8 million in 2022 corresponding to an average saving of $47,424 per patient over 2 years [^pji-pdf].
- The total direct savings (healthcare relating savings) were $71.3 million most of which was attributed to the government (63%) and private health insurers (33%). Savings were also partially attributed to patients and their families (4%).
- The total indirect savings (non-health care related savings) were $51.5 million most of which was attributed to patients and their families (67%), followed by the government (19%) and employers (14%).
- The highest saving per patients were reported for hip joints ($49,376) and patients with chronic infections ($45,131). Greater saving per patients were incurred in the first 4 years ($50,846 for year 0-2, $46,153 for year 2-4 and $25,207 for year 4-6).
These analyses will be repeated using real data in 3 years’ time and we expect this will be the first real-world cost-effectiveness data available for phage therapy.
Based on these health economics calculations, we can state that phage therapy is an efficient spend of public health dollars right now.
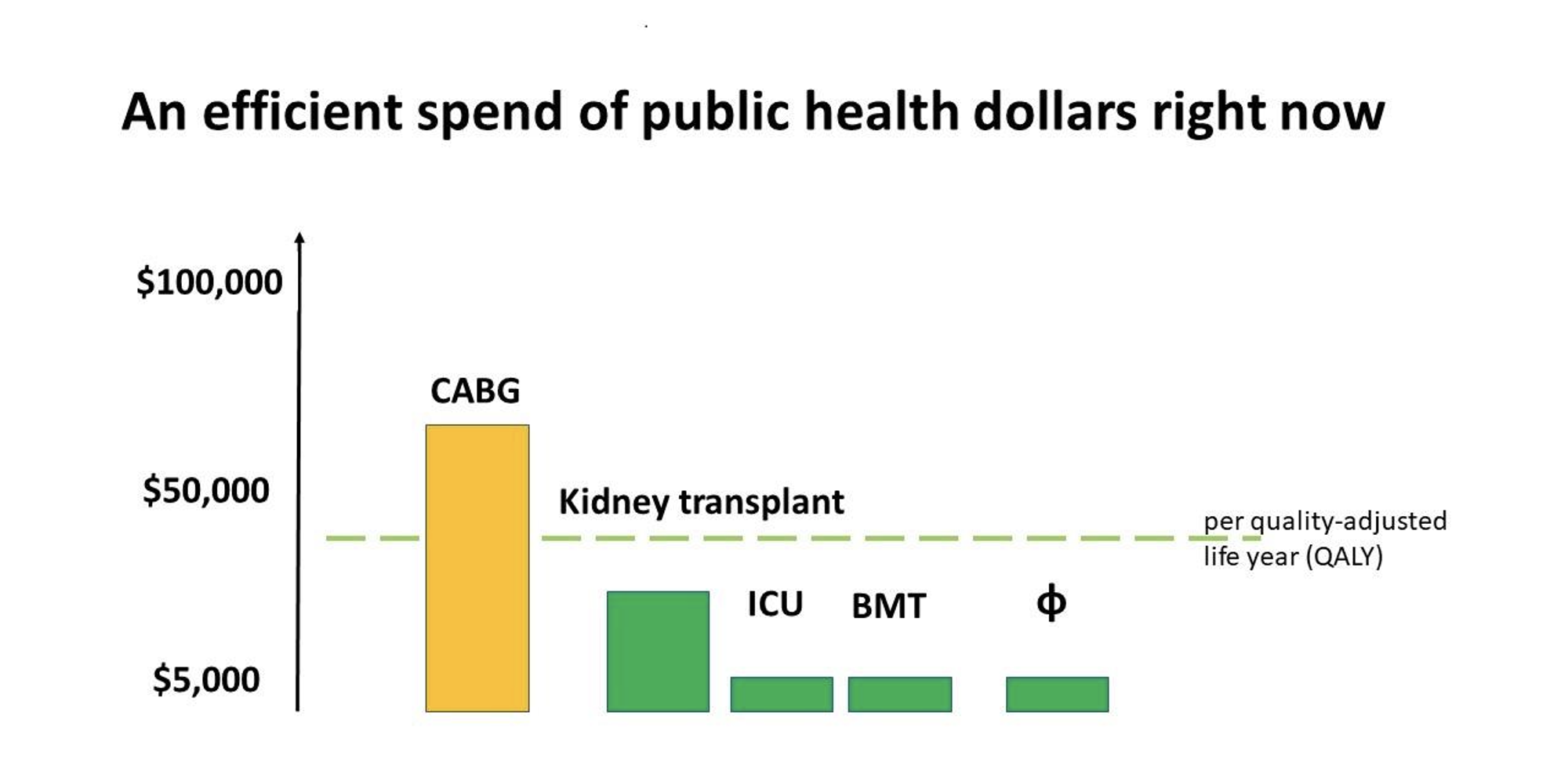
Jon Iredell reviewed the decisions by Australian government (PBS, Pharmaceutical Benefit Scheme [^14]) which indicated a willingness to pay $15,000 – $45,000 AUD for a quality adjusted life year (the quality adjusted life year is a health economist measure of return on health investment). This graph shows that ICU and bone marrow transplant services are very good value, as are kidney transplants. Coronary bypass grafting (CABG) is over $50,000 AUD. Our externally commissioned modelling showed that phage therapy to be at least as good value as bone marrow transplantation and ICU services. Importantly, this is a lot cheaper to implement.
Aligning reimbursement [^15] and regulatory policies for phage therapy is our challenge (more on this in my next blog) and phage therapy must remain under the watchful eye of research and drug safety committees for now. The Australian Antimicrobial Resistance Network – AAMRNet – has set out a position statement [^16] around funding of novel antimicrobials in Australia but this remains an open conversation.
At Phage Australia, we have scheduled for Health Technology Assessment and Market Access Analysis on Phage Therapy, in order to inform PBAC and MSAC.
A recent example of experimental therapy being accepted into all aspect of healthcare system is Novartis’ outcome-based healthcare strategy of introducing CAR-T cell therapy into the mainstream market [^17] based on one single-arm data in adults and paediatric patients.
[^12]: https://htanalysts.com.au/
[^13]: This included data from our phage therapy clinical trial: Petrovic Fabijan, A., Lin, R.C.Y., Ho, J. et al. Safety of bacteriophage therapy in severe Staphylococcus aureus infection. Nat Microbiol 5, 465–472 (2020). https://doi.org/10.1038/s41564-019-0634-z
[^amrsepsis-pdf]: Impact of Phage Therapy on AMR Sepsis, prepared by HTANALYSTS [PDF Download] https://r2.phage.directory/WIMR01_AMRSepsis_WP_FINAL_26July2022.pdf
[^pji-pdf]: Impact of Phage Therapy on Joint Infections, prepared by HTANALYSTS [PDF Download] https://r2.phage.directory/WIMR01_PJI_WP_FINAL_26July2022.pdf
[^14]: https://www.pbs.gov.au/browse/publications
[^15]: https://hbr.org/2019/10/making-life-saving-medical-treatments-more-affordable
[^16]: https://www.mtpconnect.org.au/images/AAMRNet_PositionStatement_PricingReimbursement_2022.pdf
5. A substantial target population
The patient population who would likely to benefit from phage therapy includes patients with severe infections from car accidents, burns, cardiac device, hip and knee replacement and breast implant surgeries, cystic fibrosis, and other non-hospital acquired infections.
Building on our experience and established science, clinical and industry network, the overarching vision is to establish a clinical network ready to apply phage therapeutics. Phage Australia aims to deliver an alternative to antibiotics treatment to curb the rising problems of AMR. Over the last few years and specifically last 12 months we have established a track record demonstrating that such a vision is both achievable and feasible in the immediate future.
To note, the AusPhageNet Clinical network have identified the following target populations (this is described in the MRFF Frontiers Stage 2 grant application):
| __Target scenario__ | __Clinical Trials in Stage 2__ | __Notes__ |
| Devices and Implant Infections | STAMP [^18], diSArm [^19], ACORN | STAMP - TGA SAS scheme with clinical trial framework, uncontrolled, non-randomised salvage therapy (all AusPhageNet clinicians); disarm – Armata Pharmaceutical sponsored clinical trial. |
| Resistant Gram-Negative Infections e.g., sepsis, UTI, cardiothoracic, any cohort that needs microbiological clearance endpoint | STAMP, SNAP, PhAB, ACORN | SNAP – randomised, adaptive platform to deal with |
| Cystic Fibrosis, Lung Related Infections | STAMP, CF Kids, ACORN, PhAB | CF Kids (Ameneh Khatami); PhAB – CF Adults, nebuliser formulation (Stephen Stick) |
| Renal Dialysis patients | STAMP | STAMP – oral formulation |
| Difficult to treat infections in Indigenous and Asian Patients | STAMP, PhAB, ACORN | ACORN - Acinetobacter, Pseudomonas, Klebsiella, Melioidosis ( |
[^18]: Safety and tolerability of a standardised treatment and monitoring protocol for adult and paediatric patients receiving bacteriophage therapy (STAMP) protocol is approved nationally (2021/ETH11861, 22nd December 2021), and is registered at ANZCTR, CTRN12622000181707
[^19]: https://www.prnewswire.com/news-releases/armata-pharmaceuticals-announces-first-patient-dosed-in-phase-1b2a-disarm-study-of-ap-sa02-in-adults-with-bacteremia-due-to-staphylococcus-aureus-301552450.html
6. Broad potential revenue streams.
In the last 4 years I get asked this question a lot: can phage make money?
From my perspective, phage therapy will always have a public good element but having been managing studies involving phages as well as Phage Australia’s activities in the last few years, I can identify several components of Phage Australia, with potential to generate revenue, that differentiate us from competitors, these include:
- phage manufacturing/production,
- clinical services,
- biobanking,
- companion diagnostics and
- database/data management platform
My prediction of income streams is as follows:
Income stream 1: Clinical Service
- Phage therapy sales for:
- Hospital purchases from their drug budget (government or private contracts)
- Private insurance (see Novartis strategy for CAR-T therapy [^20])
- Reimbursement (regulatory policy needs to align)
- Philanthropy
- Clinical trials
- Companion diagnostics sales
- Fees for participation in education/training courses for Phage Therapy.
The target population outlined above gives investors an idea of the market for phage (in healthcare alone). I won’t discuss pricing and reimbursement models at this stage, but I anticipate rigorous discussions of “subscription of phages provided by a government health service” vs “direct billing of a phage product, fee for service” in the near future. Such legislation would impact how we (Australia) and other jurisdictions look at funding novel antimicrobials in health services (and broader applications, See One Health Initiative by WHO [^21]).
[^20]: https://www.novartis.com/research-development/technology-platforms/cell-therapy/car-t-cell-therapy-and-beyond
[^21]: https://www.who.int/news-room/questions-and-answers/item/one-health
Income Stream 2: COST-RECOVERY for BIOBANKING SERVICES
We have a collection of phages to screen against representative pathogens. Numerous high value phages can be put forward for therapeutic purposes.
A simple cost-recovery system is normal practice amongst well established biobanks e.g., DSMZ (https://www.dsmz.de German Collection of Microorganisms and Cell Cultures GmbH) and our local Core Facility WIMR biobank (>40 biospecimen collections). For example, WIMR biobank recoups costs by providing DNA and RNA extraction services for the biospecimens held by the facility, requested by researchers.
Beyond providing phages for clinical trials outlined here (and in the MRFF Frontiers Stage w proposal), this phage collection will be made available to those with any need for bioremediation or biocontrol. Use of phages is well established in the food and agriculture industry (PhageGuard, https://phageguard.com/ for listeria management), poultry, aquaculture and diary (Proteon Pharmaceuticals, https://www.proteonpharma.com/) etc.
To note, management and governance of this vast operation will require another discussion piece. Briefly, for Phage Australia, we have adopted a governance model with a national executive committee and an independent strategic advisory committee. In the first instance, terms of reference are signed off by Phage Australia partners, bound by mutual obligations and privileged access to data and biological materials (phages and reference strains). This will evolve in due course.
Income Stream 3: PACKAGED PHAGE and BACTERIAL PRODUCTS [^22]
A large holding of phages from worldwide collections broadens the ability to screen and identify high value phages that can be put forward for therapeutic purposes. We have supported several cases in this way, i.e., 2 CF paediatric patients and 1 oncology paediatric patient requiring Mycobacterium abscessus phages and 1 paediatric patient requiring Pseudomonas phage [^23]) and could do this as a service, with appropriate recompense to external owners under licensing agreements.
In this way, material transfer and licensing agreement should allow the Phage Exchange Program to present a curated collection of phages and bacteria ready for use. This includes;
- Phages of therapeutic value. Purified phage can potentially be provided with cost-recovery through the public health system (we have worked out patient journey and are costing this out). This income stream might ideally come from government and hospital contracts as a supplier of certified phages.
- Phages (single, cocktail, natural, genetically modified or chemically modified) targeting a specific antimicrobial resistant pathogen can be sold to external customers requiring such phages. Customers identified would include research laboratories and industry. Currently there is no service of this nature in the world. A major advantage is our access to a well-curated collection of pathogens (from surveillance programs) and phages. Metadata associated with the host bacteria and phages are systematically processed (SOPs are being established and in the process of harmonising across the network), curated, tested against relevant strains, sequenced and archived.
- The pathogen collections that enable this screening of phage are also of high value to research laboratories and pharmaceutical companies who wish to test their own new antimicrobial agents.
The emergence of COVID-19 in the last 3 years has highlighted global health threat from antimicrobial resistance but at the same time presents an opportunity for the antibiotic resistance market towards growth. The global antimicrobial resistance market was valued at $9.39 billion USD in 2020, and is estimated to reach $13.8 billion USD in 2027, with a compound annual growth rate of 4.68% from 2021-2027 [^24]. WHO recognises that phage therapy offers an alternative approach to combat global AMR threat.
[^22]: ATCC (https://www.atcc.org/) and Addgene (https://www.addgene.org) both package bacteria and phage products.
[^23]: Khatami A, Lin RCY, Petrovic-Fabijan A, Alkalay-Oren S, Almuzam S, Britton PN, Brownstein MJ, Dao Q, Fackler J, Hazan R, Horne B, Nir-Paz R, Iredell JR. Bacterial lysis, autophagy and innate immune responses during adjunctive phage therapy in a child. EMBO Mol Med. 2021 Sep 7;13(9):e13936. doi: 10.15252/emmm.202113936.
[^24]: https://finance.yahoo.com/news/global-13-8-billion-antimicrobial-110900720.html
Income Stream 4: SYNTHETIC PRODUCTS
A survey of phage companies [^25] indicated that genetic modification technologies (e.g., CRISPR) have been applied to phages, bacteria and plasmids to generate novel products that are protectable by patent, e.g., Locus Biosciences, BiomX and Eligo Biosciences. Chemically modified phages (e.g., conjugated with antibiotics (Hien Duong) or other valuable molecules and genetically modified phages (e.g., muddy from Graham Hatfull) will be truly novel and therefore protectable IP of potential high value.
Manufacturing Bacterial Host Strains.
While phage is the end product of a bioprocessing pipeline, the bacterial host strains are key to successful manufacturing. For example, Jon Iredell and Kamal Kamruzzaman have develop a process of curing harmful plasmids from a bacterium that can be applied even to strains with previously uncharacterised systems [^26]. This approach can be applied to ensure that no harmful AMR plasmids are included in the production pipeline, even for phages whose main target is highly AMR strains that are normally full of such plasmids and might be otherwise difficult to produce. Any infectious diseases physicians and clinical microbiologist working at an Australian public hospital would appreciate such an approach.
A collection of such curated manufacturing bacterial host strains is potentially very valuable (specifically to satisfy regulatory requirement of a therapeutic phage production). Identifying key stakeholders in phage production, marketing and distribution are being mapped out. We believe that such a venture will be the first of its kind and will fill an unique niche in bioprocessing.
[^25]: Phage Directory: Airtable list https://airtable.com/shr8f1wbrK2hvR1an/tblCpqDQJjqyqgtj0/viw01yqq3wEoCCgie
[^26]: Kamruzzaman M, Mathers AJ, Iredell JR. A Novel Plasmid Entry Exclusion System in pKPC_UVA01, a Promiscuous Conjugative Plasmid Carrying the blaKPC Carbapenemase Gene. Antimicrob Agents Chemother. 2022 Mar 15;66(3):e0232221. doi: 10.1128/aac.02322-21. Epub 2022 Jan 10. PMID: 35007138; PMCID: PMC8923210.
Income Stream 5: PERSONALISED PRODUCTS
Another attractive aspect of personalised production of phages is the Personalised therapy approach where target selectivity allows a spectrum of antibacterial activity to be tailored for clinical use. Thus, phage combinations or ‘cocktails’ can be designed to be broadly targeted to cover a range of important likely pathogens, or highly microbe-specific phage therapy can be used to leave intact the useful non-target microbiota (‘good’ bacteria) that would normally be damaged by antibiotics.
Personalised lifestyle product (not limited to clinical use) can also be developed. For example, there are phage companies dedicated to cosmetics (acne, https://phylabiotics.com/), animal/pet health (skin infection, gut microbiome) and poultry and dairy industry.
Management of gut health is part of the lifestyle supplements industry [^27] that generates billions of dollars globally. Despite inherent poor regulation associated with this industry, I cannot help but speculate that phage products can be marketed as a preventative measure for many ailments. Scientifically, restorative effects of supplements that is relevant to gut microbiome and diet [^28] can form part of the intervention strategies in, for example, sport science (e.g., enabling peak performance in elite athletes), cardiovascular diseases that involves the gut (e.g., hypertension), neurodegenerative diseases involving the gut (e.g., Parkinson’s) etc. Use of phages as a prophylaxis on medical devices and medical textile may also be a possibility.
Current trends in phage therapy involve commercial entities assembling phage cocktails to broaden the spectrum of activities of therapeutic formulations. This presents another set of challenges around the stability of combined phages, phage competition and the problem of routinely injecting high doses of mostly inactive viral particles (since often only one member of a ‘cocktail’ like this will be active against a given strain). An effective mechanism is to quickly screen an isolate against a large bank of phages or even to produce one quickly from bioprospecting. Phage Australia has demonstrated, specifically in the last 12 months that it is feasible to quickly screen (See up-and-coming work from Stephanie Lynch on Patient Screening Workflow) and focusing on bespoke therapy by quickly matching phage to patient isolate may have demand as an alternative service.
Agricultural and veterinary applications are also potentially important. A decade ago, there were only a handful of companies specialising in bacteriophage but by 2022, a fascination with the microbiome and the rise of antibiotic resistance means that bacteriophage research and development is enjoying a renaissance.
According to Credence Industry Market Research Report (October 2018), the global bacteriophage market held $567.9M USD in 2017 and is expected to grow at compound annual growth rate of 3.9% during the forecast period from 2018 to 2026. A list of phage companies on the market with their value proposition is curated by Phage Directory [^25].
[^27]: https://www.gowellnessco.com/gut-health-supplements/
[^28]: Leigh SJ, Morris MJ. Diet, inflammation and the gut microbiome: Mechanisms for obesity-associated cognitive impairment. Biochim Biophys Acta Mol Basis Dis. 2020 Jun 1;1866(6):165767. doi: 10.1016/j.bbadis.2020.165767.
Income Stream 6: DATA
Data and product provenance is central issues in biology. As the field moves towards digitalisation [^30] we identified [^31] several enabling features such as centralised governance, standardised protocols, standardised definition (e.g., Data Dictionary used in REDcap to capture STAMP trial data) and good data management that are needed to facilitate contribution of data (clinical and lab data associated with a specific phage) and product (phage and/or bacteria, see Australia Phage Passport) to the Phage Australia biobank and data system.
An integrated platform combining Artificial Intelligence and Distributed Ledger Technology [^32] and internationally standardised quality management system (e.g., ISO9001 accreditation) can ensure seamless audit and quality assurance. This in turn boosts confidence amongst users, stakeholders and investors for a specific product. We are in the process of working out a ledger system for phage product and its companion data to address sample and data provenance. To make it fun, cryptocurrency, e.g., Phage Coin has been discussed but we proceed with caution [^33].
The data, data management system and integrated platform we are building at Phage Australia is likely to be attractive to investors. A striking example of success with data utilisation and data linkage is Tempus [^34] - a Chicago-based technology company that offers genetic testing and aggregates clinical information for cancer [^35]. Groupon’s initial investment in 2015 enabled Tempus to be valued at $8.1 billion USD after raising $200 million in equity financing and $250 million in convertible debt by December 2020. Tempus said at the time that their investors included Baillie Gifford, Google, Franklin Templeton, Novo Holdings and funds managed by T. Rowe Price Group Inc. Currently Tempus is a company valued at $3.1 billion USD and its database enables clinicians to diagnose specific cancer type (and the best specific therapy to match) in real time. There is no such venture in the infectious diseases space. Phage Australia’s effort can fill this gap.
There are also many examples of co-investment from public and private sectors [^25] to bring different streams of income into an entity by combining a physical collection of samples (e.g., a biobank) integrated with an online collection of data (decentralised databases). Sweden’s national collaboration for genomic medicine [^36] (from sequencing to clinical practice) and Scandinavia’s effort in combining public and private effort to utilise data to innovate [^37] healthcare are good examples.
Funding from MRFF Frontiers Stage 2, philanthropy and investors can expedite this whole process.
[^30]: https://www.nfx.com/post/biotech-to-techbio
[^31]: Phage Biobank: Present Challenges and Future Perspectives. RCY Lin, JC Sacher, PJ Ceyssens, J Zheng, A Khalid, JR Iredell & The Australian Phage Network. Current Opinions in Biotechnology https://doi.org/10.1016/j.copbio.2020.12.018
[^32]: Pirnay J-P: Phage Therapy in the Year 2035. Frontiers in Microbiology 2020, 11; https://www.frontiersin.org/articles/10.3389/fmicb.2020.01171
[^33]: https://fortune.com/2022/03/31/cryptocurrency-web3-skepticism-molly-white/
[^34]: https://www.tempus.com/
[^35]: https://www.cnbc.com/2020/06/17/tempus-ai-health-firm-backed-by-groupon-co-founder-hunts-coronavirus.html
[^36]: https://genomicmedicine.se/en/
[^37]: https://www.searchinglifescience.com/media/123/scandinavia-is-the-latest-genomics-hub
Income Stream 7: GENOMIC SEQUENCING
For the duration of MRFF Frontiers Stage 1, Phage Australia was fortunate to have the support of several industry partners in DNA sequencing to serve the projects within the Phage Australia network.
By partnering with AGRF and the Westmead Institute Core Facility for Genomics, we were able to validate the whole genome sequencing pipeline and turn it into a self-sustainable operation. For example, a cost-recovery model was implemented in the first instance to recoup the cost of labour and reagents from a discounted rate to Phage Australia network users for phage, bacteria and metagenome sequencing. All negotiated discounts from Stage 1 were passed on to users. Many genomic sequencing service providers use this model to be self-sustainable without much external funding e.g., Ramaciotti Centre for Genomics at UNSW. We believe this model can be grown but recognise that we are not a genomic service provider.
Genomic sequencing underpins many essential activities outlined here, in particular, biobanking, phage matching and therapeutic monitoring. Success in making this self-sustainable right at the beginning in stage 1 demonstrates the feasibility of this venture beyond the next 5 years.
Concluding Remarks
Fig. 6. outlines our proposed commercial development pathway, which again, highlights the importance of co-investment of public and private sectors.
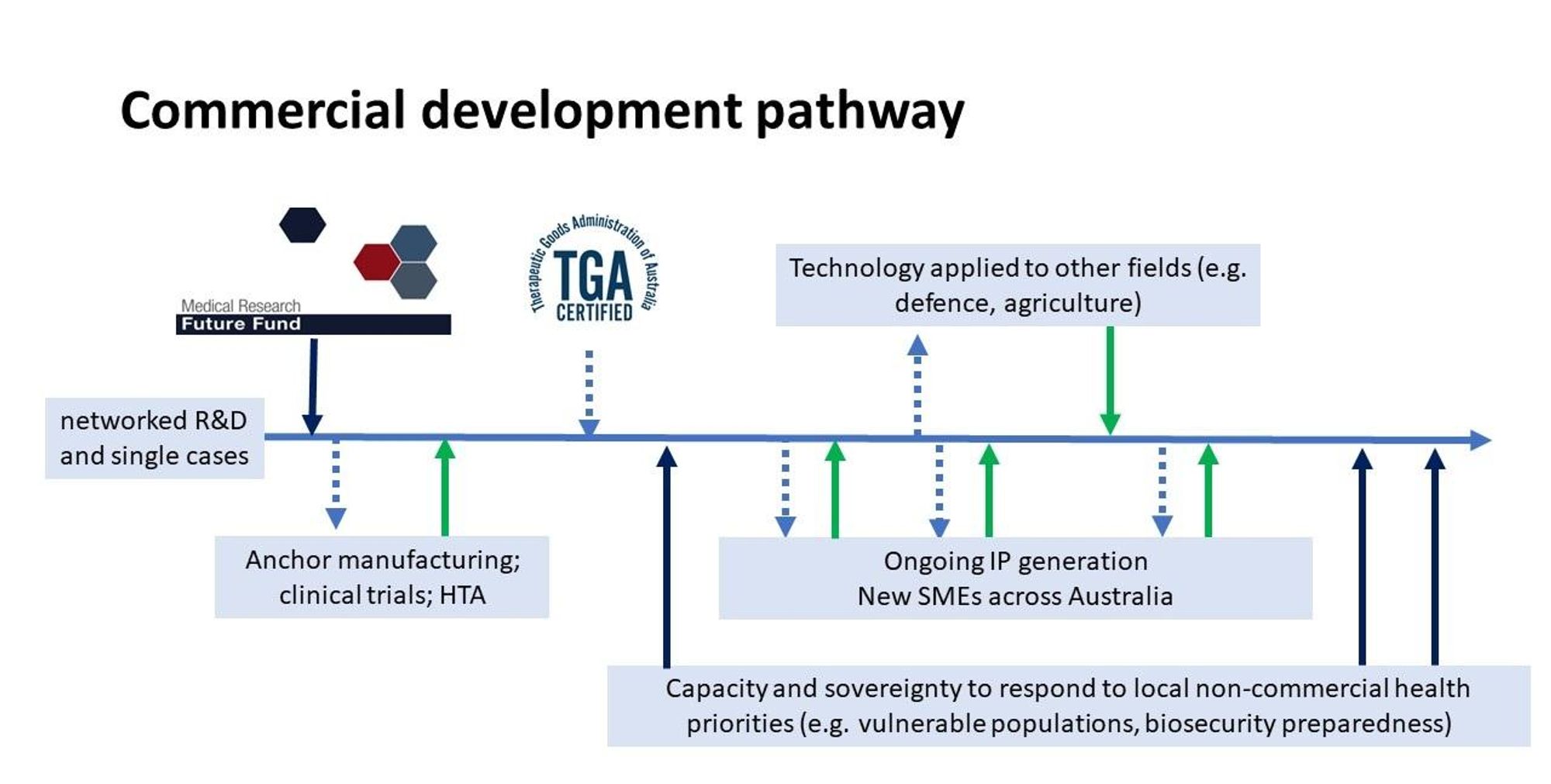
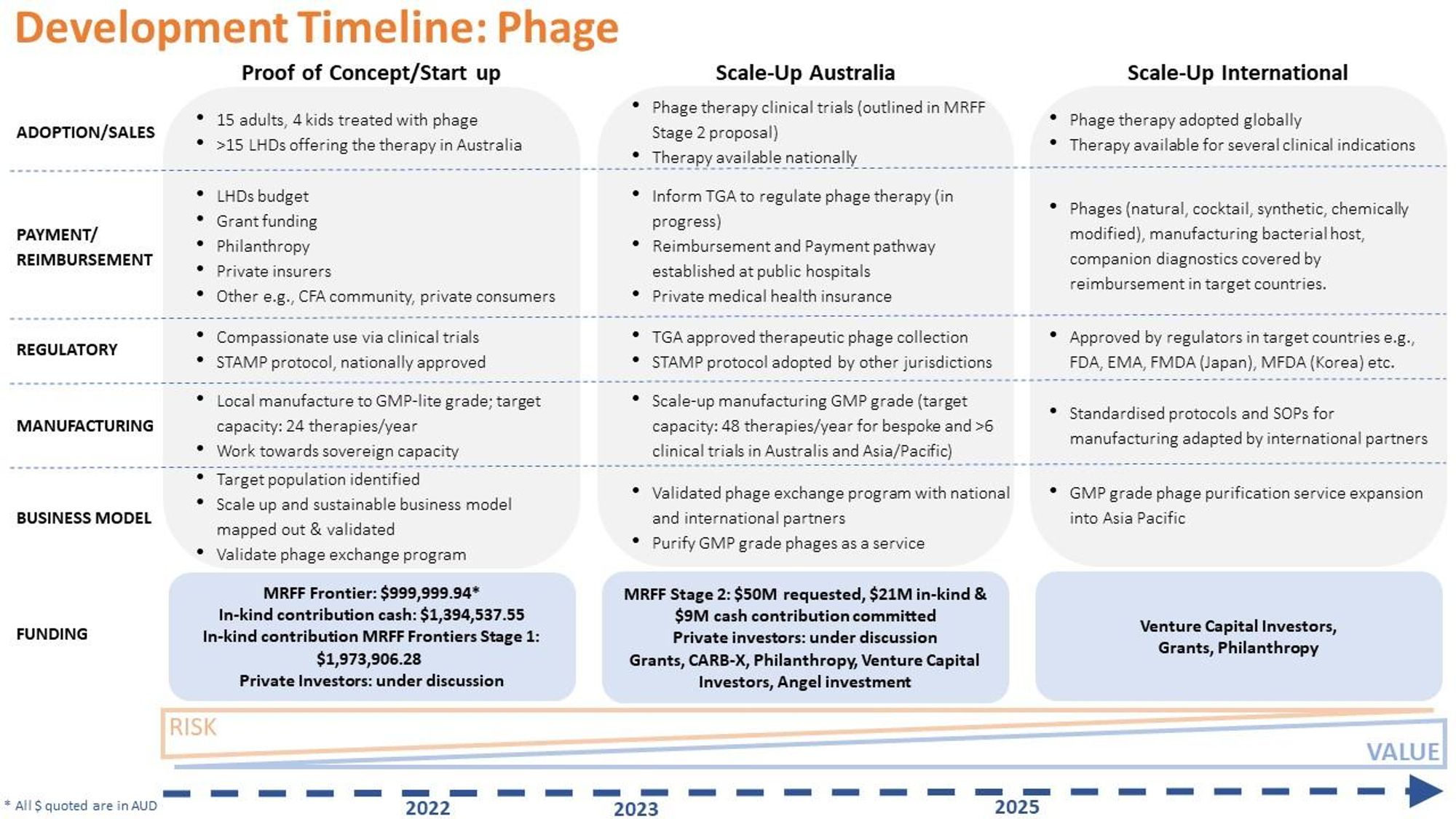
A significant challenge facing any effort to commercialise phage therapy is that phages discovered in nature cannot be patented. It is feasible, however, to identify IP (including the know-how) along this pathway including; genetically modified phages, new cocktails containing optimal combinations of phages, new antimicrobials, chemically modified phages, AMR-cured manufacturing bacterial host strains, companion diagnostics for therapeutic screening etc (see list of income streams outlined above). From my perspective, the development timeline based on the last 12 months (Fig. 7) can be projected to increase value and de-risk the challenges I have highlighted so far.
British economist Jim O’Neill was commissioned by the UK government to review AMR [^38] and he identified phages as the number 1 option to antibiotics. While it is encouraging to know that there are many new and innovative preclinical pipelines of antibacterial agents [^39] and antibiotics [^40], given the track record of antibiotics leading to AMR, phages pose as an outstanding AMR solution, and demands immediate attention and investment from both the government and venture capital.
So, can phage make money amidst all the challenges I have outlined here?
I would like to quote Stephen Stick and leave you with this thought: “Howard Florey didn’t discover penicillin but he worked out how to use it. His first thought was not “how do we make a buck out of this”? Yet the application of penicillin created a mega industry including discovery, manufacture, formulation and delivery modes.”
[^38]: O'Neill, J. (2016). Tackling Drug-Resistant Infections Globally: final report and recommendations, Wellcome Trust and UK Government.
[^39]: https://www.who.int/activities/coordinating-r-and-d-on-antimicrobial-resistance
[^40]: https://www.pewtrusts.org/en/research-and-analysis/data-visualizations/2014/antibiotics-currently-in-clinical-development
Downloads
PDF: Impact of Phage Therapy on AMR Sepsis, prepared by HTANALYSTS
PDF: Impact of Phage Therapy on Joint Infections, prepared by HTANALYSTS
Acknowledgement
- Discussion on commercialisation of phage and phage therapy: Jon Iredell, Laura Collie, Idalia Dawidowska, Viktor Windeyer, James Jones, Sam Walker, Jan Zheng, Jessica Sacher, Stephen Stick, Trevor Lithgow, Joey Lai, Bill Russell.
- Discussion on market sounding analysis of phage therapy, pathogen and phage biobanking, TGA working group and education package on phage therapy: NSW Health i.e., Tony Penna, Laura Collie, Julia Warning, Sian Hope, Patricia Morten, Anne O’Neill, Caitlin Pitt.
- Contribution to HTAnalyst reports: Jon Iredell, Ruby Lin, Ameneh Khatami, Indy Sandaradura, Tim Gilbey, Amit Shetty, Aldo Saavedra.
- Discussion on infrastructure, governance and operations of Phage Australia: Jon Iredell, Mark Rees, Nicholas McKay, Mark Mclean, Phage Australia executives.
- Discussion on ethics, patient screening, phage exchange, genomics workflow, biobanking and surveys: Jon Iredell, Stephanie Lynch, Joey Lai, Jessica Sacher, Brian Gloss, Jan Zheng, Lani Atwood, Anthony Kicic, Nouri Ben Zakour, Ruwani Dissanayake, Steve Petrovski, Nicki Mileham, Martin Plymoth, Ameneh Khatami, Holly Sinclair, Shinwon Lee.
- Discussion on international phage biobanking, phage exchange and AMR network: Heejoon Myung, Pieter-Jan Ceyssans, Jean-Paul Pirnay, Tobi Nagel, Ben Temperton, Graham Hatfull, Greg German, Stephanie Lesage, Richard James, Richard Alm, Ronen Hazan, Ran Nir-Paz.
- Special thanks to the research support team at the Sydney University: Ed Hendriks, Nicole Makoviney, Kailing Wang, David Boyd.
To cite the health economics report:
Phage Australia. Impact of Phage Therapy: AMR Sepsis. 2022. Available from: https://dl.phage.directory/WIMR01_AMRSepsis_WP_FINAL_26July2022.pdf.
Phage Australia. Impact of Phage Therapy: Prosthetic Joint Infections. 2022. Available from: https://dl.phage.directory/WIMR01_PJI_WP_FINAL_26July2022.pdf.
To cite this white paper:
Lin, RCY. Westmead Institute for Medical Research (2022). Phage Australia - building a sustainable ecosystem for phage therapy. Retrieved from https://phageaustralia.org/blog/sustainable-phage-therapy
NB: Please feel free to write to me with your thoughts. I extend a challenge out to entrepreneurs and intrapreneurs to help us refine business plans and business models.